Gynecomastia is defined as the benign hypertrophy of the male mammary glands, usually caused by abnormal hormonal changes in the body.
How Common Is Gynecomastia in Men?
Gynecomastia occurrence within specific age groups:
Over 65% of male newborns (up to 90%) present increased mammary tissue, due to transfer of maternal and placenta hormones – the symptoms naturally receding after a few weeks.
At ages 12 – 14, about 60% of the boys get gynecomastia, usually generated by a slow or delayed release of testosterone in the body, a temporary increase of aromatase (an enzyme which acts as a catalyst for the conversion of testosterone into estradiol) or sensitivity towards estrogens.
As puberty hits, sudden releases of several specific growth hormones stimulate testosterone production and gynecomastia disappears naturally, within a time frame of one or two years.
Between the ages of 16 to 20, the percentage lowers to 19%, followed by an increase up to 40% for male patients aged between 25 and 45.
About 60% of the men above 50 years old present increased mammary tissue, due to declining testosterone levels.
Mammary hypertrophy caused by fat tissue (in case of obesity) is called pseudogynecomastia and it’s treated with Gynetrex system which comprises of a healthy diet, workouts and dietary supplement.
Non Physiological Gynecomastia
This type of gynecomastia is generally associated with diseases or medication that go along with low testosterone levels, an accented conversion of testosterone into estrogen, high levels of estrogen.
Body builders who use high amounts of androgens (the enzyme aromatase will convert testosterone into estrogen).
Patients who are in treatment for prostate cancer have a higher predisposition for developing gynecomastia (up to 60%), while those who are in treatment for benign prostate hypertrophy are almost in the clear (about 1%).
A high amount of estrogens can be found in certain creams, body lotions and other types of cosmetics.
Other products known to trigger gynecomastia are based on lavender oil and tea tree, because they contain substances that inhibit androgens.
It takes only a couple of months for the symptoms to disappear, once the usage of those products has been interrupted.
Diagnosing gynecomastia and further medical investigations
The diagnosis is made taking in consideration multiple factors:
– A physical exam, where the physician pays attention to the size and consistency of the mammary tissue, possible nipple retraction, nipple pain, mammary secretion, axillary adenopathy – which could indicate the presence of breast cancer.
– History – lump growth speed, any association with liver or kidney illnesses, hyperthyroidism, testicular insufficiency, family history of gynecomastia and/or breast cancer.
Patients with physiological, pubertal or asymptomatic gynecomastia don’t need further medical investigation, although a reevaluation is recommended after six months.
However, a more comprehensive assessment is needed for those patients who:
– Have macromastia (lumps bigger than 5 cm);
– Experience tenderness, pain;
– Notice nipple retraction, mammary secretions;
– Have noticed an accelerated growth of the mammary tissue;
– Have discovered the presence of hard lymph nodes.
The usual procedures are mammography, breast biopsy, testicular and breast ultrasound and specific laboratory tests.
Male Breast Cancer
Male breast cancer is a rare disease – less than 1% of all breast cancer cases are related to men.
Some of the risk factors are:
– Growing old – the average age for men with breast cancer has been established around 68 years old;
– High estrogen levels (due to hormonal medication, obesity, estrogen exposure from food, cosmetics, certain body building food supplements, liver dysfunction);
– Klinefelter syndrome (double or multiple X chromosomes and a single Y chromosome instead of the normal single X, single Y chromosomes specific to male DNA);
– Family history of breast cancer;
– Radiation exposure – for instance, radiation therapy to the chest in order to treat Hodgkin’s disease for patients under 30 years old or other types of radiation, for long periods of time.
Symptoms of male breast cancer:
– Nipple pain, nipple retraction; soreness or discoloration in the nipple area;
– Mammary secretion;
– Large or hard lymph nodes under the arm.
If the mammogram and/or breast ultrasounds have indicated the possibility of cancer, a biopsy will be performed. If the cancer has been certified, further tests will be done in order to determine the type and stage of cancer.
Treatment For Male Breast Cancer
The treatment is the same as for female patients; it depends on the stage of development – which refers to its size and whether it has already spread or not, at the moment of the diagnose.
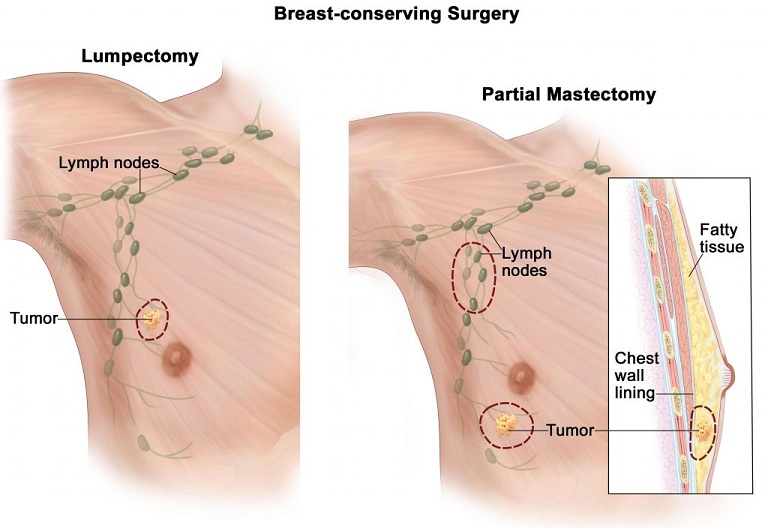
The usual procedures are:
– Surgery – the removal of the breast (mastectomy);
– Chemotherapy – after surgery, in certain circumstances (the patient is young; the tumor was larger than 2 cm; cancer cells present in the lymph nodes);
– Radiotherapy – also after surgery, to reduce the risk of the cancer coming back;
– Hormone therapy if the tests have shown that the cancer cells have hormone receptors;
– Biological therapy if the tests show the cancer cells to have HER2 receptors (human epidermal growth factor receptor 2).
Conclusion
Because male breast cancer is a rare occurrence, men usually aren’t aware of its possibility.
There is an objective need for an increased public awareness of male breast cancer.
Ignorance causes a high rate of mortality among male patients with breast cancer, because the diagnosis is made too late, when the tumors are large and after the cancer has spread in the body.
As it holds good for all cancer types, the sooner it is discovered, the higher chances are that treatment may prove successful.
Therefore, regular checkups are important – keep in touch with your physician and make sure you let them know about any irregularity in the breast area – or under the arm (lumps, pains, hard tissue as presented above).